Dr. Methodius Isaac Bonkers, M.D.
Bonkers Institute for Nearly Genuine Research
bonkersinstitute.org
If no symptoms appear about the stomach, nor the blood be misaffected, and fear and sorrow continue, it is to be thought the brain itself is troubled, by reason of a melancholy juice bred in it, or otherwise conveyed into it, and that evil juice is from the distemperature of the part, or left after some inflammation. – Charles Lepois, 1618
For centuries, mental illness was believed to be caused by fumes or vapors rising upwards toward the brain from the stomach or other organs of the body, but today mental disorders are widely believed to originate from chemical imbalances produced within the brain itself.
Gone are the days of darkness and superstition, when madness was blamed on black biles, wicked spirits and evil juices. Thanks to recent advances in neuropsychiatric bioscience (and relentless advertising by pharmaceutical manufacturers) we now know that mental illness is an organic physical medical condition, disease, disorder, syndrome or functional deficit of some kind stemming from a combination of biological, environmental and/or genetic factors which may be linked to specific abnormalities, disruptions, imbalances, structural defects and clinically measurable, observable or hypothetical levels of neurotransmitter function within the basal ganglia, hippocampus, thalamus or adjacent regions of the encephalon, situated inside the cranial cavity occupying the intracranial space underlying the skull and outer surrounding membrane.
With each passing decade, our knowledge has increased and our vocabulary has grown to include a multitude of polysyllabic words which help doctors describe the origin and etiology of mental illness in ways that sound more scientific than ever before, as the following graph illustrates:
| LENGTH OF WORDS USED TO EXPLAIN MENTAL ILLNESS, 1600 - 2005 | |||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Syllables per word: | |||||||||||||
| 1 - | Fumes | ||||||||||||
| Vapors | |||||||||||||
| 3 - | Dopamine | ||||||||||||
| Serotonin | |||||||||||||
| 5 - | Norepinephrine | ||||||||||||
| Hydroxytryptamine | |||||||||||||
| 7 - | Selenomethionine | ||||||||||||
| Adrenocorticotropin | |||||||||||||
| 9 - | Dihydroxyphenylalanine | ||||||||||||
| Imidazolonepropionase | |||||||||||||
| 11 - | Methylenedioxymethamphetamine | ||||||||||||
| Year: | 1600 | 1945 | 2005 | ||||||||||
A systematic review of the relevant literature reveals that modern medical neuroscience has progressed from 3-syllable words to 11-syllable words in less than five hundred years. Even more impressive than the ever-expanding vocabulary of mental health professionals is the ever-growing number of mental disorders diagnosed and treated by them.
In the early 19th century, four categories of mental illness were recognized by medical science: dementia, hysteria, mania, and melancholia. The landscape changed dramatically in 1952 when the American Psychiatric Association (APA) published its Diagnostic and Statistical Manual (DSM) listing 106 distinct mental disorders. Subsequent DSM revisions have reflected the APA's willingness to embrace, diagnose and treat newly-discovered mental disorders, often coinciding with the introduction, marketing and promotion of newly-patented pharmaceutical products:
|
DSM-1, 1952: 106 disorders DSM-II , 1968: 185 disorders DSM-III, 1980: 265 disorders DSM-IV, 1994: 357 disorders |
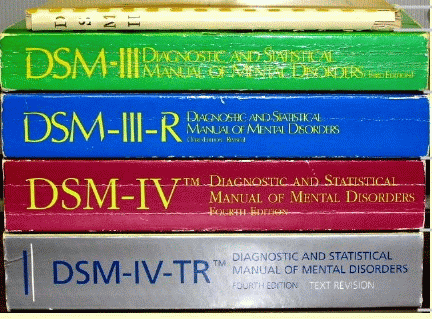 |
How many diseases there are, is a question not yet determined; Pliny reckons up 300 from the crown of the head to the sole of the foot: elsewhere he saith, morborum infinita multitudo, their number is infinite. Howsoever it was in those times, it boots not; in our days I am sure the number is much augmented. -- Robert Burton, 1621
With the DSM, the APA lends legitimacy to the proliferation of mental disorders, greatly expanding the market for new prescription drugs. This mutually beneficial relationship between the drug industry and the APA has grown increasingly transparent in recent years, with neither side unduly concerned about the appearance of ethical impropriety, conflict of interest, or violation of public trust.
Thanks in part to a 3-way alliance formed by the APA, pharmaceutical manufacturers and the federal government, the line between drug promotion and disease promotion is now virtually nonexistent. A perfect example is the Food and Drug Administration's approval of Sarafem® for the treatment of premenstrual dysphoric disorder (PMDD). Seeking a new source of revenue following Prozac's patent expiration, pharmaceutical giant Eli Lilly simply changed the name of the drug from Prozac to Sarafem and changed the color of the pill from green to pink, targeting a new market that was created by the inclusion of PMDD in DSM-IV.
Similar examples of government-approved disease mongering by drug companies and the APA include:
- Ritalin® approved for attention deficit disorder;
- Paxil® approved for social anxiety disorder;
- Wellbutrin® approved for seasonal affective disorder;
- Requip® approved for restless legs syndrome;
- Cymbalta® approved for diabetic nerve pain associated with olanzapine;
- Lyrica® approved for chronic invisible ailment of unknown origin (fibromyalgia);
- and the list goes on...
A principal objective of modern medical science is the discovery of new medications, but the rapid pace of pharmaceutical innovation has resulted in a corresponding need for the discovery of new diseases as well. Organizations like the APA play a crucial role: as long as the drug industry continues to develop new products, the APA guarantees a steady supply of new diseases requiring treatment.
Until now, newly-minted diseases have multiplied almost as quickly as newly-patented pharmaceutical products. However, continual reliance on the discovery, invention and fabrication of entirely new and distinct discrete disease entities may prove impractical in the near future, given the sheer volume of new drug patents every year. This has necessitated a shift in focus toward the re-classification of multiple manifestations of single clinical entities through the creation of entirely new subcategories, comorbidities, prodromal forms of combined clinical subtypes, shadow syndromes and the like. A major breakthrough in this process was the introduction of the all-purpose diagnostic catch-all category known as Not Otherwise Specified, or NOS, which is applied whenever the symptoms of any given mental disorder appear to fall within the larger category but do not meet the criteria of any specific disorder within that particular category.
For example, the current edition of the DSM divides the disease formerly known as manic depression into two categories, Bipolar I and Bipolar II, then subdivides these two broad categories into a variety of distinct sub, sub-sub, and sub-sub-sub categories including Dysthymic, Cyclothymic, Manic, Hypomanic, Mild, Moderate, Severe, Single Episode, Recurrent, Full or Partial Remission, With or Without Psychotic Features, and so on, before arriving at the one-size-fits-all diagnosis of Bipolar Disorder Not Otherwise Specified, reserved for patients whose symptoms fail to match any of the previous categories.
The disease formerly known as dementia praecox is now called schizophrenia and it is also subdivided by type: Paranoid, Disorganized, Catatonic, Undifferentiated, Residual, Schizoaffective, Schizophreniform, Delusional or Psychotic. If the symptoms of a precociously demented patient fail to meet the criteria for any of the preceding categories, the diagnosis "Psychotic Disorder Not Otherwise Specified" may be utilized with clinical precision and supreme confidence that Medicaid will pay for it.
Personality disorders are classified as Paranoid, Schizoid, Schizotypal, Obsessive-Compulsive, Histrionic, Antisocial, Narcissistic, Avoidant or Borderline, depending how severely the clinician is annoyed by the patient. When something about the patient's attitude rubs us the wrong way but we're uncertain how to label it, a diagnosis of Personality Disorder Not Otherwise Specified will suffice.
As can be seen, the category "Not Otherwise Specified" greatly enhances the mental health professional's ability to successfully diagnose, treat, label and permanently stigmatize any patient whose illness might otherwise slip through the screening examination undetected – potential clients who would fall under the radar, bypassing the social safety net and tragically escaping the warm loving embrace and abundant therapeutic benefits of our nation's glorious mental health system.
The current edition of the Diagnostic and Statistical Manual identifies a limited number of diagnostic entities, diseases, disorders, syndromes, dysfunctions, pathologies and conditions within the Not Otherwise Specified (NOS) category. These include:
- Adjustment Disorder NOS
- Adverse Effects of Medication NOS
- Alcohol-related Disorder NOS
- Amnestic Disorder NOS
- Amphetamine-Related Disorder NOS
- Anxiety Disorder NOS
- Anxiolytic-Related Disorder NOS
- Attention-Deficit Hyperactivity Disorder NOS
- Bipolar Disorder NOS
- Caffeine-Related Disorder NOS
- Cannabis-Related Disorder NOS
- Cocaine-Related Disorder NOS
- Communication Disorder NOS
- Conduct Disturbance NOS
- Delirium NOS
- Dementia NOS
- Depressive Disorder NOS
- Disorder of Infancy, Childhood, or Adolescence NOS
- Disruptive Behavior Disorder NOS
- Dissociative Disorder NOS
- Dyssomnia NOS
- Eating Disorder NOS
- Factitious Disorder NOS
- Hallucinogen-Related Disorder NOS
- Hypnotic-Anxiolytic-Related Disorder NOS
- Impulse-Control Disorder NOS
- Inhalant-Related Disorder NOS
- Learning Disorder NOS
- Mood Disorder NOS
- Movement Disorder NOS
- Nicotine-Related Disorder NOS
- Opioid-Related Disorder NOS
- Other Substance-Related Disorder NOS
- Paraphilia NOS
- Parasomnia NOS
- Parent-Child Problem NOS
- Personality Disorder NOS
- Pervasive Developmental Disorder NOS
- Phobia NOS
- Psychogenic Disorder NOS
- Psychotic Disorder NOS
- Relational Problem NOS
- Sedative-Anxiolytic-Related Disorder NOS
- Sexual Disorder NOS
- Sleep Disturbance NOS
- Somatoform Disorder NOS
- Tic Disorder NOS
- Unknown Substance-Related Disorder NOS
It must be remembered the above listing is only partial and does not include every human condition known to exist, nor every single condition ever experienced by anyone who ever lived, nor every conceivable condition which might someday affect someone now living or yet to be born.
Most clinicians agree NOS (Not Otherwise Specified) is preferable to NEC (Not Elsewhere Classified) simply because it sounds more authoritative. The skilled artisan will recognize that there are alternative nomenclatures, nosologies, and classification systems for pathologic psychological conditions and that these systems evolve with medical scientific progress.
If you require a more exact division of these ordinary diseases which are incident to men, I refer you to physicians; they will tell you of acute and chronic, first and secondary, lethales, salutares, errant, fixed, simple, compound, connexed, or consequent, belonging to parts or the whole, in habit, or in disposition, etc. – Robert Burton, 1621
We are all somehow dreadfully cracked about the head, and sadly need mending. – Herman Melville, 1851
To be continued...
© 2013 Bonkers Institute for Nearly Genuine Research